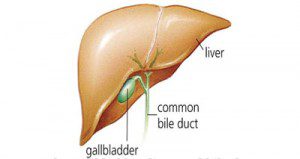
Gallbladder is a pear-shaped organ attached to the under surface of the liver. Its main function is to collect and store bile (a digestive liquid) produced by the liver. After eating, the gallbladder contracts and releases the bile. The bile is carried via a small tube called the cystic duct and then larger tubes called bile ducts into the small intestine where it helps in the digestion.
Gallstones are solid clumps of cholesterol or pigment material that form in the gallbladder. When the concentration of bile components like cholesterol or bile pigments increases, they precipitate to form solid crystals. These crystals then stick together and form gallstones. Why some people form gallstones is not clearly known, and therefore there is nothing one can do or avoid in the diet to prevent the gallstones from forming.
Gallstones are usually diagnosed by a relatively simple test called ultrasonography. In this test a jelly is applied to the skin and a probe is moved over the abdominal wall to capture images of the internal organs.
Not all patients who have gallstones require surgery. In most instances those who do not have any symptoms (silent gallstones) may not require treatment. However, a decision not to operate should be taken only after consulting a specialist because when left alone gallstones are likely to cause complications.
Once a patient develops symptoms because of gallstones they do not go away on their own. Some patients can be temporarily managed with medicines or by making dietary adjustments, such as cutting down on fat intake. However, this treatment is not a permanent solution to the problem. Treatment with homeopathic or ayurvedic medicines is never able to dissolve gallstones. Taking these types of medicines in the hope that the gallstones will “melt away” carries the risk of the patient developing serious complications. Surgical removal of the gallbladder (cholecystectomy) is the best treatment for patients in whom the gallstones cause symptoms.
It is important to understand that a gallbladder that forms gallstones is a diseased organ and is not functioning normally. Therefore removal of such a diseased gallbladder is not associated with any side effects. Over a period of time, the function of storage of bile is taken over by the bile ducts and there is no impairment of the digestive process.
In the past, the gallbladder was removed by making a large incision on the abdomen (open cholecystectomy). This incision invariably caused a lot of pain after the operation and as a result the patient had to stay in the hospital for about week. Even after discharge the overall recovery required several weeks. The risk of infection was higher in this larger incision.
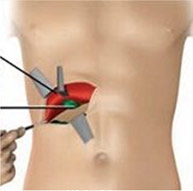
How is the gallbladder operation performed around the world today?
Today, all over the world the removal of gallbladder is performed by laparoscopic cholecystectomy. Instead of a fifteen to twenty cm incision of an open operation, the laparoscopic cholecystectomy is carried out through four small punctures each of which is ? to 1 cm in length. As the incisions are small, the pain after the operation is minimal and therefore the recovery is much faster. The chances of infection in the incisions are almost negligible.
It is important to note that laparoscopic cholecystectomy is a major operation performed under general anaesthesia. The surgeon passes a cannula (a narrow tube) into the abdomen in the region of the umbilicus. A telescope connected to a camera is passed inside the abdomen through the cannula. The camera is connected to a television monitor so that a magnified view of the patient’s internal organs appears on the screen. The surgeon and his team conduct the operation by observing the television screen. The surgeon then inserts other cannulas and passes long, thin instruments inside the abdomen through them. Using these instruments the gallbladder is separated from its attachments and is removed through one of the openings. After removal of the gallbladder, the small incisions are closed with a few stitches.

Patient Experience
My troubles with gallbladder stones
I had two seemingly isolated episodes of severe stomach pain and nausea–coincidentally both times while on business trips away from home, during the night in hotel rooms – once in Mumbai (2007) and then again in Chennai (early 2008).
Gallbladder surgery: a big deal?
I was detected with gallstones in 2010 and being a doctor I knew that I would require a surgery as I was getting symptoms. The decision to get the surgery done was easy and I went to Dr Deepraj Bhandarkar at Hinduja Hospital.
A doctor’s tryst with an infected gallbladder
One Monday morning I woke up feeling out of sorts. As Mondays are busy days, I decided to pull myself together and get to work. I conducted a full OPD and went for my coffee break with friends.
In a small proportion of patients (1% – 3%) during the operation the surgeon may decide to convert the laparoscopic operation to a traditional open one.This is required if the organs cannot be visualized safely or handled effectively. Conversion to an open operation is never considered a complication. In fact, it reflects a sound judgment on the part of the surgeon who is interested in safeguarding the patient’s safety.
The patient does experience some amount of pain for about 12 to 24 hours after laparoscopic cholecystectomy depending on individual tolerance. Also, some nausea and vomiting is not uncommon in the first 12 hours. Patients are always given medications to relieve the pain and take care of the nausea. Usually, the patient is allowed to drink fluids within 6 to 8 hours of surgery and is able to have meals from the day after surgery. Activity is dependent on how the patient feels, but all patients are encouraged to get up and walk as soon as they are comfortable. Most patients go home within a 48 hours after laparoscopic cholecystectomy as compared to five to seven day following the traditional open operation. Some patients, particularly the elderly and those with other medical problems like diabetes may have to stay in the hospital a little longer. In general, patients recover completely within 7 to 10 days.
In our society patients often prefer to take things easy for weeks after any operation because of a fear that they may harm themselves by being active. After laparoscopic cholecystectomy the recovery is quite rapid. Soon after returning home the patients are allowed all activities they feel comfortable with. Depending on the nature of their job, most patients are able to return to work within ten to fifteen days following a laparoscopic cholecystectomy. Patients with light, desk jobs usually return in a few days while those involved in heavy lifting may require a little more time.
While there are risks associated with any kind of operation, the vast majority of patients undergoing laparoscopic cholecystectomy experience no complications. It is important to remember that before undergoing any type of surgery – whether laparoscopic or traditional it is important to make sure that the surgeon performing the operation is well trained and experienced. In the hands of such surgeons the risks of laparoscopic cholecystectomy are negligible.
- Less pain from the small incisions after surgery
- Shorter hospital stay – usually overnight
- Shorter recovery time
- Faster return to normal diet
- Faster return to work or normal activity
- Better cosmetic healing
https://www.sages.org/publications/patient-information/patient-information-for-laparoscopic-gallbladder-removal-cholecystectomy-from-sages/
http://emedicine.medscape.com/article/1582292-overview
Publications and abstracts
- Bhandarkar DS. A simple method of securing a cholangiography cannula. Trop Doct 1993; 23: 175.
- Udwadia TE, Patil SU, Udwadia RT, Bhandarkar DS. Laparoscopic cholecystectomy in India. Int Surg 1992; 77: 149-53.
- Bhandarkar DS. Laparoscopic fenestration of nonparasitic liver cysts. Surgery 2000; 4:34-37.
- Bhandarkar DS, Shah RS. Intrahepatic hematoma – a rare complication of laparoscopic cholecystectomy. Surg Endosc 2004; 18:869.
- Bhandarkar DS, Shah RS. Laparoscopic choledochoduodenostomy for retained bile duct stone J Postgrad Med. J Postgrad Med 2005; 51:156-7.
- Udwadia TE, Bhandarkar DS, Bhirangi KS, Bhoyar SV. Laparoscopic cholecystectomy is feasible, safe and complete surgically, greatly beneficial economically. Indian J Gastroenterol 1990; 9: A11.
- Udwadia TE, Bhandarkar DS, Patil SU, Udwadia RT. Laparoscopic cholecystectomy in developing countries. Indian J Gastroenterol 1991; 10: A76.
- Udwadia TE, Udwadia RT, Bhagat GJ, Patil S, Bhandarkar DS. Laparoscopic cholecystectomy in the developing world. Surg Endosc 1994;8:432.
Book chapters
- Bhandarkar DS. Laparoscopic cholecystectomy: pearls and pitfalls. In, Workshop Proceedings on Biliary-pancreatic Diseases, 2001
Presentations, invited lectures & videos
- Udwadia TE, Bhandarkar DS, Bhirangi KS, Bhoyar SV. Laparoscopic cholecystectomy is feasible, safe and complete surgically, greatly beneficial economically. Annual Conference, Indian Association of Gastroenterology, Bombay, 1990.
- Bhandarkar DS, Udwadia TE. Peritoneoscopy in liver disease – a surgeon’s viewpoint. Overseas Meeting, Royal College of Surgeons of Edinburgh, Bombay, 1991.
- Udwadia TE, Bhandarkar DS, Patil SU, Udwadia RT. Laparoscopic cholecystectomy in developing countries. Annual Conference, Indian Association of Gastroenterology, Bombay, 1991.
- Bhandarkar DS, Udwadia TE. Peritoneoscopy in malignancy. Annual Conference, Research Society of J.J. Hospital, Bombay, 1991.
- Udwadia TE, Bhandarkar DS, Patil S, Udwadia R. Laparoscopic cholecystectomy in developing countries. 3rd World Congress of Endoscopic Surgery, Bordeux, 1992.
- Udwadia TE, Udwadia RT, Bhagat GJ, Patil S, Bhandarkar DS. Laparoscopic cholecystectomy in the developing world. 4th World Congress of Endoscopic Surgery, Kyoto, 1994.
- Bhandarkar DS. Laparoscopic fenestration for simple hepatic cysts. 3rd Congress of Endoscopic Surgery, Hyderabad, 1998.
- Bhandarkar DS. Laparoscopic transcystic bile duct exploration. 44th Annual Conference, International College of Surgeons, Indore, 1998.
- Bhandarkar DS. Laparoscopic treatment of nonparasitic hepatic cysts. Annual Conference of Maharashtra Chapter of ASI, Akola, 1999.
- Bhandarkar DS. Laparoscopic cholecystectomy – role of the endoscopist. ‘Clinical Challenges in Biliary–Pancreatic Endoscopy’, Mumbai, 2000.
- Bhandarkar DS, Punjani RM, Bhanushali HS, Pradhan C. Laparoscopic management of hepatic cysts. Annual Conference of Maharashtra Chapter of ASI, Nasik, 2002.
- Bhandarkar DS, Punjani RM. Laparoscopic management of hepatic cysts. 5th Annual Conference of IAGES, Kolkata, 2002.
- Bhandarkar DS. Laparoscopic hepatopancreatobiliary surgery. Update Laparoscopic Surgery- Expanding Horizons, Mumbai, 2003.
- Bhandarkar DS. Laparoscopic surgery for bile duct stones. International Forum on Minimally Invasive Surgery, Beijing, 2004.
- Bhandarkar DS, Shah RS. Laparoscopic choledochoduodenostomy for a retained bile duct stone. Annual Conference of Maharashtra Chapter of ASI, Thane, 2004.
- Bhandarkar DS. Laparoscopic choledochoduodenostomy. International Forum on Minimally Invasive Surgery, Beijing, 2004.
- Shankar M, Bhandarkar DS, Shah RS, Udwadia TE. Laparoscopic exploration of the bile duct and its primary closure over stent ASIAPACIFICON 2005, Mumbai, 2005.
- Bhandarkar DS. Mechanisms of bile duct injury at laparoscopic cholecystectomy. National Congress of AMASI, Kolkata, 2006.
- Shankar M, Bhandarkar DS, Katara AN, Udwadia TE. Laparoscopic cholecystectomy in the elderly: a valid option? ELSA 2007, Hyderabad, 2007.
- Bhandarkar DS, Katara AN, Udwadia TE. Towards safer laparoscopic cholecystectomy – Ten Commandments. ELSA 2007, Hyderabad, 2007.
- Bhandarkar DS, Katara AN, Kochar R, Udwadia TE. Laparoscopic exploration of the bile duct with its primary closure. MASICON 2008, Kolhapur, 2008.
- Bhandarkar DS. Detection and management of CBD stones in the era of laparoscopic cholecystectomy. 5th FIAGES Course, Pune, 2009.
- Mittal G, Bhandarkar DS, Shah RS, Katara A, Udwadia TE. Feasibility and safety of single incision laparoscopic cholecystectomy in acute cholecystitis. MASICON 2011, Mumbai, 2011.
- Ghuge A, Bhandarkar D, Kapadia K, Trivedi DR. Predicting difficulty of laparoscopic cholecystectomy. MASICON 2011, Mumbai, 2011.
- Bhandarkar DS. Laparoscopic cholecystectomy – making it safe. Dombivali Kalyan Surgeon’s Association, Kalyan, 2011.
- Bhandarkar DS. Laparoscopic cholecystectomy: A to Z. CME on Complications, Sholapur Surgical Society, Sholapur, 2011.
- Bhandarkar DS. Management of bile duct stones in the laparoscopic era. 23rd FIAGES Course, Aurangabad, 2012.