Lymph nodes are small, bean-shaped glands throughout the body. They are part of the lymphatic system, which carries fluid (lymph fluid), nutrients, and waste material between the body tissues and the bloodstream. The lymphatic system is an important part of the immune system, the body’s defense system against disease. The lymph nodes filter lymph fluid as it flows through them, trapping bacteria, viruses, and other foreign substances, which are then destroyed by special white blood cells called lymphocytes.
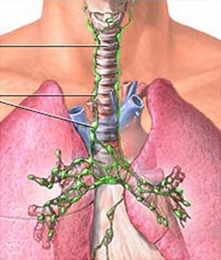
Lymph nodes may be found singly or in groups. And they may be as small as the head of a pin or as large as an olive. Groups of lymph nodes can be felt in the neck, groin, and underarms. They are also present throughout the chest adjacent to all the blood vessels to and from the internal organs.
The main causes of enlargement of the lymph nodes in the chest are:
- A bacterial illness including tuberculosis
- Cancer, such as leukemia, Hodgkin’s disease, and non-Hodgkin’s lymphoma
- Lung cancer
- Sarcoidosis
Enlarged lymph nodes inside the chest are usually suspected and diagnosed when tests such as a chest-ray or a CT scan are carried out during an illness such as fever for which no obvious cause is found (pyrexia of unknown origin). The patient may also have symptoms such as cough, diminished appetite or weight loss. In addition, the doctor may order certain blood tests to find out the cause of the enlarged lymph nodes.
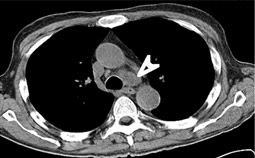
As many diseases cause the lymph nodes in the chest to be enlarged and there is no certain way of knowing which disease is causing them to be enlarged doctors often require a small sample (biopsy) from the lymph nodes to make a clear diagnosis. Only after the diagnosis can the treated be started.
If along with enalarged lymph nodes in the chest there are lymph nodes in easily accessible areas such as the neck, under the armpits or groin doctors often get a needle sample from these (called fine needle aspiration cytology or FNAC) and send it to a pathologist. For diagnosis of certain diseases, e.g. lymphoma, the pathologist requires a large piece of the lymph node (biopsy). The biopsy may be carried out under local or general anaesthesia depending on the site of the enlarged nodes and patient and surgeon preference.
In patients who only have enlarged lymph nodes in the chest but no nodes elsewhere that can be easily biopsied, the situation is slightly different. It may be possible to biopsy lymph nodes at some locations inside the chest under the guidance of a CT scan. The doctor pass a fine needle to the area of the enlarged lymph nodes under local anaesthesia as the area is being monitored on a CT scanner.
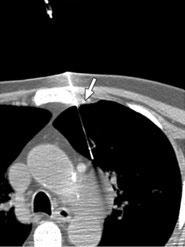
Sometime the sample obtained using a CT guided biopsy is too small for the pathologists to give a definite diagnosis of the cause of enlarged lymph nodes. In some patients the enlarged lymph nodes may be located so close to important blood vessels or internal organs that it is risky to attempt putting a needle into them under CT guidance.
Traditionally such patients required an open operation on the chest to obtain a sample from the lymph nodes. Today many of the enlarged lymph nodes in the chest that cannot be biopsied under CT guidance (which is naturally the preferred method) patients can have a thoracoscopic biopsy of the lymph nodes.
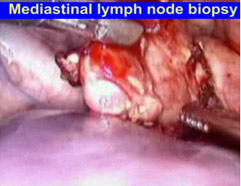
Thoracoscopic lymph node biopsy is carried out under general anaesthesia. The surgeon makes a small (about 1-cm) incision and places a short tube called a cannula in the chest. To look inside the chest, the surgeon passes a telescope connected to a miniature video camera through the cannula. The telescope that picks up the picture of the inside of the chest and transmits it to a television screen. The surgeon then exposes the area of enlarged lymph nodes and obtains a biopsy with the help of special, long instruments introduced inside the chest through two other cannulas and by observing the picture of the operative site on the television screen. At the end of the procedure a small tube may be placed in the chest.
Usually the sample is sent to a pathologist immediately for processing (called frozen section) when the patient is under anaesthesia. This helps the surgeon, as the pathologist is able to indicate whether or not the sample is adequate and also is able to point to a tentative diagnosis. The final diagnosis often takes five to seven days as the sample has to be processed in a particular manner and special tests carried out on it. In case the sample is deemed inadequate the surgeon can obtain more samples before the patient is brought out of anesthesia.