A lung biopsy is usually performed to determine the cause of abnormalities, such as shadows or nodules that appear on chest x rays. It can confirm a diagnosis of cancer, especially if malignant cells are detected in the patient’s sputum or bronchial washing. In addition to evaluating lung tumors and their associated symptoms, lung biopsies may be used to diagnose lung infections, especially tuberculosis and Pneumocystis pneumonia, drug reactions, and chronic diseases of the lungs such as sarcoidosis, interstitial lung disease and pulmonary fibrosis.
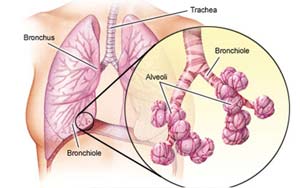
The biopsy can be performed in 4 ways. The method used depends on where the sample needs to be taken from and the patient’s overall health.
- Bronchoscopic biopsy: This is usually performed under mild sedation by giving an intravenous medicine to make you sleepy and relaxed. The doctor passes a lighted instrument (bronchoscope) through the mouth or nose and into the airway and removes a sample of lung tissue. This method may be used if an infectious disease is suspected, if the abnormal lung tissue is located next to the breathing tubes (bronchi), or before trying more invasive methods, such as an open lung biopsy.
- Needle biopsy: A needle biopsy uses a long needle inserted through the chest wall (under local anaesthesia) to remove a sample of lung tissue. This method is used if the abnormal lung tissue is located close to the chest wall. A computed tomography (CT) scan, an ultrasound, or fluoroscopy is usually used to guide the needle to the abnormal tissue.
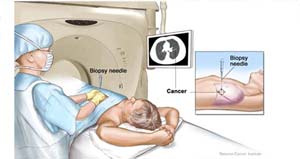
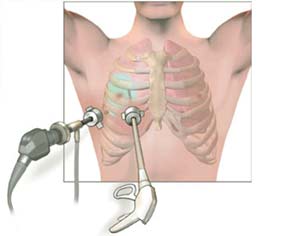
- Open lung biopsy: This is performed under general anaesthesia. The surgeon makes a cut (incision) between the ribs and removes a sample of lung tissue. An open biopsy is usually done when the other methods of lung biopsy have not been successful, cannot be used, or when a larger piece of lung tissue is needed for a diagnosis.
Usually the sample is sent to a pathologist immediately for processing (called frozen section) when the patient is under anaesthesia. This helps the surgeon, as the pathologist is able to indicate whether or not the sample is adequate and also is able to point to a tentative diagnosis. The final diagnosis often takes five to seven days as the sample has to be processed in a particular manner and special tests carried out on it. In case the sample is deemed inadequate the surgeon can obtain more samples before the patient is brought out of anaesthesia.