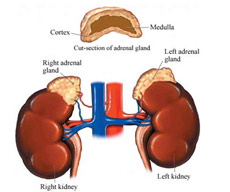
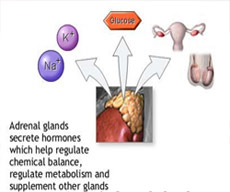
The adrenal glands are small organs located above each kidney. A normal adrenal gland is triangular in shape and roughly the size of one’s thumb. The function of the adrenal glands is to produce hormones. These hormones are responsible for various functions in the body such as control of blood pressure, levels of various chemicals in the blood, use of water in the body, usage of glucose and the “fight or flight” reaction during times of stress. The hormones produced by the adrenal glands include cortisol, aldosterone, epinephrine and norepinephrine and a small amount of sex hormones estrogen and androgen).
 |
 |
Patients with adrenal gland problems may experience a variety of symptoms related to the excess hormone/s produced by the abnormal gland. Some tumors may not produce any symptoms and grow to a large size by the time they are diagnosed.
Cortisol producing tumors: Tumors that produce an excess of hormone cortisol cause a syndrome termed Cushing’s syndrome. Patients suffering from Cushing’s syndrome develop obesity (especially of the face and the mid-body), high blood sugar, high blood pressure, menstrual irregularities, fragile skin, and prominent stretch marks. Only when the tests indicate that the tumor is situated in the adrenal gland does removal of the adrenal gland become necessary.
Aldosternaomas: These are tumors that produce an excess of hormone called aldosterone. Patients may suffer from a raised blood pressure and often have low levels of potassium in the blood. The low potassium levels can result in symptoms of weakness, fatigue and frequent urination.
Pheochromocytomas: These are tumors that produce excess of hormones called “catecholamines”. The patient may experience very episodes of high blood pressure characterized by severe headaches, anxiety, palpitations, excessive sweating and rapid heart rate. These spells may last from a few seconds to several minutes.
Incidentalomas: An adrenal mass or tumor may sometimes be found when a patient gets an abdominal ultrasound or CT scan for evaluation of another problem. Such tumors are called “incidentalomas”. An incidentaloma may be any of the above types of tumors, or may produce no hormones at all.The patient needs to be evaluated to check whether or not the tumor is producing excess hormones. When an incidentaloma causing no symptoms and the tests indicate that it is not producing excess hormones and is benign, it does not need to be removed. Surgical removal of an incidentaloma is required only if:
- The tumor is found to produce excess hormones
- Is more than 4-5 centimeters in diameter
- If, based on the scans, there is a suspicion that the tumor could be cancerous.
Adrenal gland cancers: These are called adrenocortical cancers and are rare. They are usually very large at the time of diagnosis and require an open operation for their removal.
If a patient is suspected to have an adrenal tumor based on his/her symptoms, doctors recommend certain blood and urine tests to check if there is excessive production of hormones. The next step is to carry out tests like a CT scan, MRI scan or MIBG scan to determine the precise location of the tumor. Rarely, a test called selective venous sampling may be necessary.
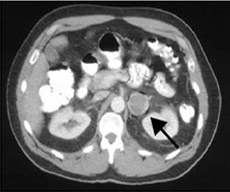 |
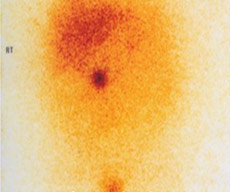 |
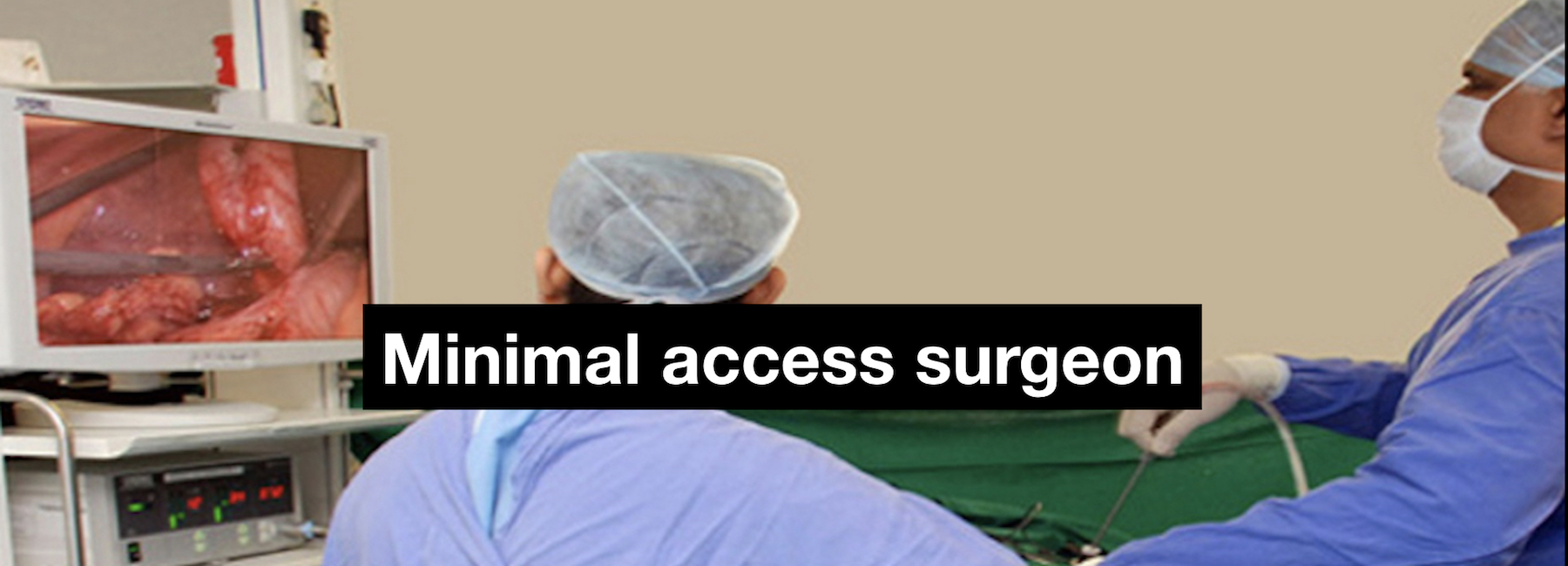
When a patient is found to have an adrenal tumor producing excess hormone/s or is suspected to be cancerous, surgical removal of the tumor is the preferred treatment. Suspected cancerous tumors are removed by open surgery through an 8-10 inch incision in the flank or in the upper part of the abdomen. Most other tumors are ideally removed by laparoscopic surgery.

Before hospitalization
- Patients with Cushing’s syndrome need to receive extra doses of cortisone medication on the day of surgery and for a few months afterwards until the other (retained) adrenal gland has resumed normal function.
- Patients with an aldosteronoma may need to have their serum potassium checked and take extra potassium if the level is low. The blood pressure needs to be controlled.
- Patients with a pheochromocytoma will need to be started on special medications several weeks prior to surgery to control their blood pressure and heart rate.
In a small number of patients the laparoscopic method cannot be performed. In that situation, the operation is converted to an open procedure. Factors that may increase the possibility of choosing or converting to the “open” procedure may include:
- Obesity
- A history of prior abdominal surgery causing dense scar tissue
- Inability to visualize the adrenal gland clearly
- Bleeding problems during the operation
- Large tumor size (over 8 or 10 cm in diameter)
The decision to perform the open procedure is a judgment decision made by your surgeon either before or during the actual operation. When the surgeon feels that it is safest to convert the laparoscopic procedure to an open one, this is not a complication, but rather sound surgical judgment. The decision to convert to an open procedure may be required in order to ensure patient safety.
- After laparoscopic adrenal gland removal, most patients return to their room. Occasionally, patients with a pheochromocytoma may require admission to an intensive care unit after surgery to monitor their blood pressure. Most patients can de discharged from the hospital within two or three days after surgery.
- Patients with an aldosterone-producing tumor will need to have their serum potassium level checked after surgery and may need to continue to take medications to control their blood pressure.
- Patients with cortisol-producing tumors and Cushing’s syndrome will need to take prednisolone or cortisol pills after surgery. The dose is then tapered over time as the remaining normal adrenal gland resumes adequate production of cortisol hormone.
- Patients are encouraged to engage in light activity while at home after surgery. Patients can generally shower the day after the operation.
- Post-operative pain is generally mild and controlled with painkiller medication.
- Most patients can resume normal activities, including driving, walking up stairs, light lifting, and work within 10 – 15 days.
- Less pain from the incisions after surgery
- Shorter hospital stay
- Shorter recovery time
- Faster return to normal diet
- Faster return to work or normal activity
- Better cosmetic healing
- Reduced risk of herniation and wound problems, particularly in patients with Cushing’s syndrome who have poor healing as a result of increased levels of cortisol
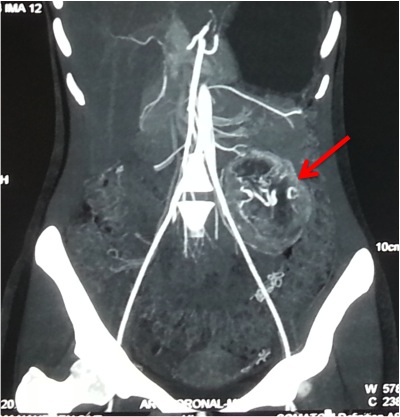
- Bhandarkar DS. Laparoscopic adrenalectomy. Bombay Hosp J 2005; 47:356-58.
- Bhandarkar DS, Katara A, Mittal G, Udwadia TE. Laparoscopic management of renal hilar pheochromocytomas. Surg Laparosc Endosc Percutan Tech 2012;22:148-151.
- Bhandarkar D, Mittal G, Katara AN, Behera RR. Laparo-endoscopic single-site left adrenalectomy using conventional ports and instruments. Urol Ann 2014;6:169-172.
Presentations, invited lectures & videos
- Katara AN, Bhandarkar DS, Shah RS, Udwadia TE, Chadha M. Laparoscopic left adrenalectomy for pheochromocytoma. Annual Conference of Maharashtra Chapter of ASI, Thane, 2004.
- Katara AN, Bhandarkar DS, Udwadia TE. Dislodgement of clips from adrenal vein during laparoscopic adrenalectomy. Endosurgery 05, New Delhi, 2005.
- Shankar M, Bhandarkar DS, Shah RS, Udwadia TE. Laparoscopic adrenalectomy: preliminary experience. ASIAPACIFICON 2005, Mumbai, 2005.
- Bhandarkar DS, Behera RR, Katara AN, Udwadia TE. Laparoscopic resection of pheochromocytomas situated in the renal hilum. AMESCON 2012, Dubai, 2012.
- Bhandarkar DS. Laparoscopic adrenalectomy. Medical and Surgical Endocrinology Update, Mumbai, 2005.
- Bhandarkar DS. Laparoscopic adrenalectomy for pheochromocytoma. Inter-hospital Scientific Meet on Hypertension, Mumbai, 2005.
- Bhandarkar DS, Katara AN, Udwadia TE. Comparative laparoscopic anatomy of the adrenal glands. ELSA 2007, Hyderabad, 2007.
- Bhandarkar DS, Katara AN, Kochar R, Chauhan P, Kapadia F, Purandare V. Laparoscopic adrenalectomy for extra-adrenal pheochromoccytoma. 54th Annual Conference of International College of Surgeons. Trichy, 2008.
- Bhandarkar DS. Adrenal diseases: open versus laparoscopic surgery. Seminar on Endocrine Surgery: Current Scenario, Mumbai, 2009.
- 1Bhandarkar DS. Laparoscopic surgery for benign adrenal diseases – the new gold standard. Annual Conference of the International College of Surgeons – Indian Section, Amritsar, 2009.
- Mittal G, Bhandarkar DS, Katara AN, Udwadia TE. Laparoscopic resection of extra-adrenal pheochromocytoma. 9th Biennial Congress of IAGES, New Delhi, 2010.
- Bhandarkar DS, Mittal G, Katara A, Chauhan P, Udwadia TE. Laparoscopic resection of extra-adrenal pheochromocytomas. ELSA2011, Singapore, 2011.
- Bhandarkar DS. Laparoscopic adrenalectomy for a large left pheochromocytoma. ELSA2011, Singapore, 2011.
- Bhandarkar DS. Single incision laparoscopic adrenalectomy. Annual Conference of IASO, Mumbai, 2010.
- Mittal G, Bhandarkar DS, Katara A, Udwadia TE. Laparo-endoscopic single-site left adrenalectomy. MASICON 2011, Mumbai, 2011.
- Bhandarkar DS, Mittal G, Katara A, Udwadia TE. Laparo-endoscopic single-site adrenalectomy. ELSA2011, Singapore, 2011.
- Bhandarkar DS, Behera RR, Katara AN, Udwadia TE. Laparo-endoscopic single-site left adrenalectomy. AMESCON 2012, Dubai, 2012.
- Bhandarkar DS. Laparoscopic adrenalectomy – why, when and how? 6th International Congress of Society of Laparoscopic Surgeons of Bangladesh, Dhaka, 2012.
- Bhandarkar DS. Adrenal incidentaloma. Postgraduate CME of Jaslok Hospital, Mumbai, 2013.
- Bhandarkar DS. Approach to a patient with incidentally detected adrenal mass. Continuing Surgical Education Series of Somaiya Hospital, Mumbai, 2013.
http://endocrinediseases.org/adrenal/incidentaloma.shtml
http://endocrinediseases.org/adrenal/surgery.shtml
http://endocrinediseases.org/adrenal/pheochromocytoma.shtml
http://endocrinediseases.org/adrenal/paraganglioma.shtml